
I can’t remember what started first, the heart palpitations or the nightmares, or exactly when it all began. I thought it was grief. I thought it was the anxiety I’d been born with, or a physical expression of the emotional turmoil I’d been thrown into.
Last year was the worst year of my life, because it’s been a condensed, amplified version of everything that has defined previous tough times — worsening chronic illness, losing loved ones and experiencing setbacks so constant that it’s almost comedic. I write books about those very things, and I think the universe constructed this year to make sure that I never run out of inspiration.
I could explain it month by month, how I had gallbladder surgery in January 2025, cared for my grandmother through her two surgeries in February, and had another procedure myself in March. Then, that same grandmother went on hospice in April and passed away in May.
By late May, I went to see my trusted primary care provider, and I told her I thought I needed my anxiety medication adjusted. She listened, and she agreed, but she told me she never likes to blame physical symptoms on anxiety. Looking back, her philosophy of care was life-changing.
So, I walked out of there with a heart monitor that I wore for three weeks. It showed that my heart rate got up to 180 while I sat watching a local production of “Waitress,” singing my actual heart out in flagrant violation of theater etiquette.
I saw a cardiologist who said it seemed like I’d been in fight-or-flight mode for months, and that was almost ironic in hindsight. After that, I started on a beta blocker that was incredibly effective at stabilizing my heart rate. It was the first hit of relief I’d felt in months, but as the volume of my pounding heart lowered, I could finally hear the noise of my other symptoms.
I settled into a new rhythm, one where my heart was calmer but everything else was increasingly chaotic. By my birthday in August, I was getting used to the vivid, recurring nightmares I began having of plane crashes and feeling myself burning alive. They started out centered around my grandmother, and that’s why I blamed them on grief. The death rattle is haunting, and I knew I’d never forget hearing it come from her throat, so I wasn’t surprised that it echoed in those wild dreams. But then other people started to die in my dreams, too — my parents, my brother, my sister’s elderly dog.
The plane crashes weren’t new. They’ve served as a particularly violent symbol in my dreams for years — especially during college finals weeks and just before job interviews — but I have never once been on the plane. I would just watch it fall out of the sky. Sometimes it landed on a familiar building. Sometimes I’d be waiting at the airport to pick up someone I love, and I saw them explode. Those dreams don’t require much analysis, because I’ve always known that what I fear isn’t my own death, it’s losing those close to me.
But then I began to die — over and over again — in my dreams. And I always burned, whether it was an incendiary car accident or a tragic building fire where I took everyone down with me. Everything was so realistic, I swear I could smell the smoke, I could feel the flames on my face, and I’d always wake up drenched in sweat.
Courtesy of Marissa Eller
Even once I was awake, the heat never let up, and I’d break out in these weird hyperthermic episodes all throughout the day. I was nauseous, and my appetite was unpredictable. I woke up each day never knowing how I’d feel, whether I’d stay awake for 24 hours or need to nap by noon.
My routine was interrupted by sudden, intermittent pain that was both severe and different from any I’d ever had. Those episodes would start with a vague, crampy feeling in my side that radiated to my back. It would then spike into something entirely unmanageable — quick bursts of agony, like lightning bolts striking me. They’d pass as fast as they came, but they left lingering soreness and lingering questions.
My shape changed, especially the outline of my constantly enflamed face. My mood continued to tank, and I was overwhelmed by equal parts pure anxiety and the unsettling feeling that something just wasn’t right. I no longer recognized myself mentally, physically or emotionally.
I thought it might be easier to just get to know the new person I was becoming. I could learn to love her racing heart and her transformed frame and her puffy, red face, but I knew that I would never get used to her mind.
The cavernous recesses of my brain are the only place that I’ve ever been comfortable, and I had to fight to keep that safe space.
I had a follow-up appointment with my primary care provider scheduled on my birthday, and I did what everyone tells you not to do: I went searching. I did my own research, looking for any bread crumbs that I could piece together into a path from my new unrecognizable self.
In the end, it was an accident, really. I got lucky. I found a year-old abdominal CT report from the first time I went to the ER with inexplicable pain, and it read: “There is a stable 1 cm left adrenal nodule that previously demonstrated attenuation values consistent with benign lipid rich adenoma on noncontrast CT of 1/25/2016.”
No one had told me about it at that time, and I certainly hadn’t known about it since 2016.
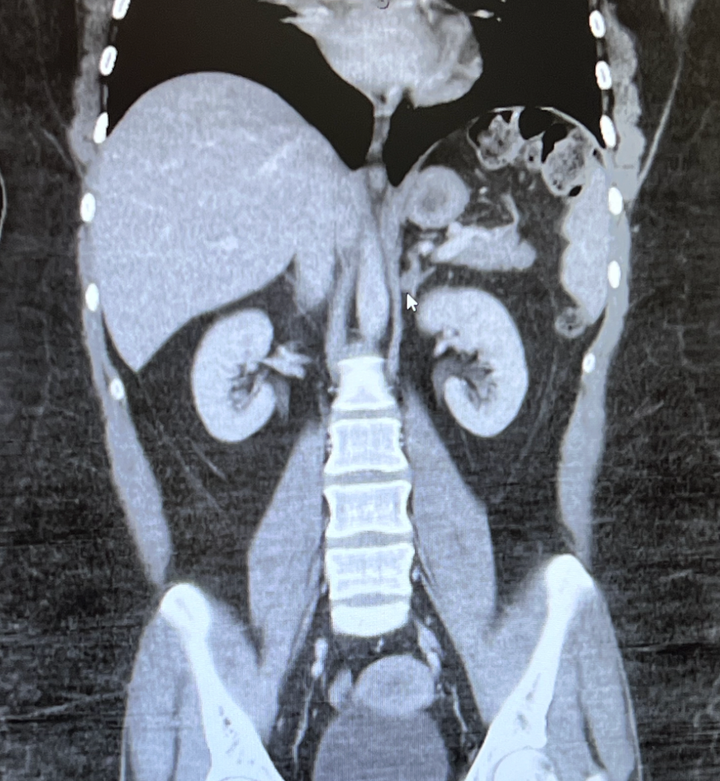
Courtesy of Marissa Eller
I dove into the trenches of the internet to learn more about adenomas and how they can secrete their own hormones. My PCP, the kind of practitioner who would rather squeeze you in for a same-day visit than send you to urgent care or the ER, said that could explain everything.
She mentioned something called Cushing’s syndrome, which is a disorder caused by long-term exposure to cortisol, a hormone made by the adrenal glands. Cortisol is known as the stress hormone, and it plays a role in things like heart rate, blood pressure, blood sugar, metabolism, and the body’s sleep-wake cycle. Tumors, like adrenal adenomas, can make their own cortisol, wreaking havoc on nearly all of the body’s systems.
“Why do my patients have to tell me these things?” My PCP muttered in frustration as she typed in a request to have the scans sent over. To my surprise, her disbelief didn’t lie with me, but the lack of continuity of care I’d received. I watched her regain her composure as she turned from the computer to face me directly, and then she explained the procedure she wanted me to undergo.
I’d have to take a steroid that night — one singular dexamethasone pill — between 11 p.m. and midnight. I’d then come back the next morning and get my blood drawn between 7 and 9 a.m. In people with typical functioning, the steroid would suppress the adrenal glands, and morning cortisol levels would be extremely low — near zero. If the mass on my adrenal gland was secreting hormones, that wouldn’t be the case. It would refuse to be suppressed.
As I waited for the results, I had another episode. I don’t know what else to call them. I ended up in the ER again, and a new scan showed the nodule had grown some, and it was now “indeterminate” — whatever that meant.
Still, no one told me. I read about it in the report, just like I had before. My mom made me call and get an ER follow-up appointment with my PCP as soon as I could, and she saw me the next morning. My bloodwork had finally come back, and my cortisol level was three times too high.
“You have Cushing’s,” she said, rather simply. It was almost anticlimactic after this yearslong comedy of errors.

Courtesy of Marissa Eller
She referred me to a doctor who specialized in endocrine surgery an hour away, because sending patients to the nearest medical school is what you do in suburban North Carolina when things get serious.
I panicked like never before, and I blamed it on the mass itself, because it was almost literally making its own anxiety. I kept thinking that the specialist would tell me the bloodwork was wrong, and the mass wasn’t making hormones, and it was nothing to worry about, let alone treat.
I called the hospital to request the CT images from 2025, 2024 and 2016 to bring with me to the appointment. Remember how I said this was a comedy of errors? They couldn’t find the images or the report from 2016 and claimed I never had a CT scan there that year. I now have no idea from where the radiologist pulled the information they compared against my 2024 CT scan, if those images were mine or if they even ever existed.
“How long have you known about the nodule?” the endocrine surgeon asked me during my first appointment at the big, scary hospital.
“Depends on who you ask,” I said. I tried to explain the missing images and report, and I told him no one had actually ever mentioned the mass to me — I’d discovered it myself by reading my write-ups.
He was amazing, and he showed me the images. The mass looked like a fuzzy little mold spore sitting on top of my left kidney. My mom took pictures of the screen because she knew I’d want them. We talked about my symptoms, and he told me the agonizing episodes that sent me to the ER were likely kidney stones, a short-term complication of the effects of cortisol.
The surgeon said leaving the mass alone to keep overproducing hormones would be detrimental to my health in the long term, especially because I’m not even 30. The tumor was the size of a Skittle, but it could end up causing myriad problems, including heart attacks, blood clots, muscle weakness and broken bones.
He recommended removing the mass and my left adrenal gland, and he wanted to look at my scars from the gallbladder surgery I’d had in January to see how they’d healed. He looked, and he said the purpling of my incisions was caused by the excess cortisol. I was floored. He literally could confirm what was happening just by looking at me, and he actually wanted to do something about it. Six weeks later, he did.
Courtesy of Marissa Eller
When I woke up from surgery, it was remarkably quiet.
Not literally. There were shoes squeaking against the floor and the chatter of patients and staff and the sound of beds being wheeled down the hall, as well as an incessant beeping that I later learned meant my blood pressure was critically low. But the voice in my head was nearly silent. I hadn’t realized how loud my anxiety had been until that peaceful post-surgery quiet left my ears ringing.
My PACU nurse — whose name I desperately wish I knew — brought me up to my room, where my parents had been waiting the two hours it took them to stabilize me, and I heard them talking about how I still seemed to be in so much pain. My nurse told them how I couldn’t have any more pain medication because of my blood pressure, and how I’d already needed three doses of Levophed to keep it up. She called me a “tough cookie.”
I didn’t feel tough at all — not in that moment and not once during the entire miserable night where I lay flat and willed my blood pressure to rise enough to stop the beeping. Sometime in the early morning, it finally did.
A couple of hours later, an attending endocrinologist, a fellow and a few medical students came in to tell me my cortisol test from that morning had been abnormal, and that drop from an excess of cortisol to a startling low had caused the crash I’d experienced overnight.
I was going to need hormone replacement therapy for at least a month to wean my body off of the extra cortisol. Cushing’s was rare, the students were told, and it usually takes much longer to diagnose. They said I had a great PCP. It was something I already knew but a fact worth repeating.
“Have you noticed your cheeks press up against your glasses?” the fellow asked, gently, maneuvering his words carefully as we discussed my appearance.
“I have,” my mom answered from the corner of the room.
The students learned about my changed face, altered proportions, purple scars, and the flushing, sweating and heart palpitations. I wanted to tell them about the noise — the panic, the nightmares, the incessant blaring of anxiety I’d felt for months — but I was enjoying the brand-new quiet too much to disrupt it with any real rational thought. They sent me on my way with my new daily steroids and two follow-up appointments. Now, I have a new appreciation for teaching hospitals, transdermal nausea patches and adequate blood pressure.
I’m finally back where I belong — inside my own head. I’m alone there, safe and sound without the blaring noise. It’s quiet almost to the point of boredom, and I like it that way. Even if it takes years for everything else to settle down, those recesses that were once filled with relentless anxiety are now occupied by intense gratitude. What I previously viewed as a comedy of errors, I now see as an example of my own privilege. In a deeply flawed medical system where so many people are either intentionally or subconsciously ignored, even self-advocacy is an advantage not all are afforded. I had the support of my family, friends and a group of incredible health care providers who had my best interests at heart. I wouldn’t trade that for anything — not even to have symmetrical adrenal glands again.
Marissa Eller is a novelist with chronic pain and an abundance of emotions. She holds a BA in English from the University of North Carolina at Pembroke and an MFA in writing from Lindenwood University that she uses in her work as an academic consultant and adjunct professor of English. She resides in Hickory, North Carolina, with her family and two rescue cats, all of whom she couldn’t love more if she tried. When not writing, reading or helping students, she can be found thinking entirely too much about her favorite TV shows, obsessing over a band she’s loved since she was 15 or enjoying an afternoon nap. She is the author of YA novels “Joined At The Joints” and the forthcoming “Left On Read.”
Do you have a compelling personal story you’d like to see published on HuffPost? Find out what we’re looking for here and ***@******st.com.” data-vars-item-type=”text” data-vars-unit-name=”69adf6bbe4b0c722e1e5c181″ data-vars-unit-type=”buzz_body” data-vars-target-content-id=”https://www.huffpost.com/entry/mailto:pi***@******st.com” data-original-string=”dSyqfWPIns4ErGpDH06JSA==6f6Ns5EDhJpqPVIq9Azq9VMI7dp0sA05ODe4LKVUMggcvM=” title=”This contact has been encoded by Anti-Spam by CleanTalk. Click to decode. To finish the decoding make sure that JavaScript is enabled in your browser.” data-vars-target-content-type=”url” data-vars-type=”web_external_link” data-vars-subunit-name=”article_body” data-vars-subunit-type=”component” data-vars-position-in-subunit=”1″>send us a pitch at pi***@******st.com.






